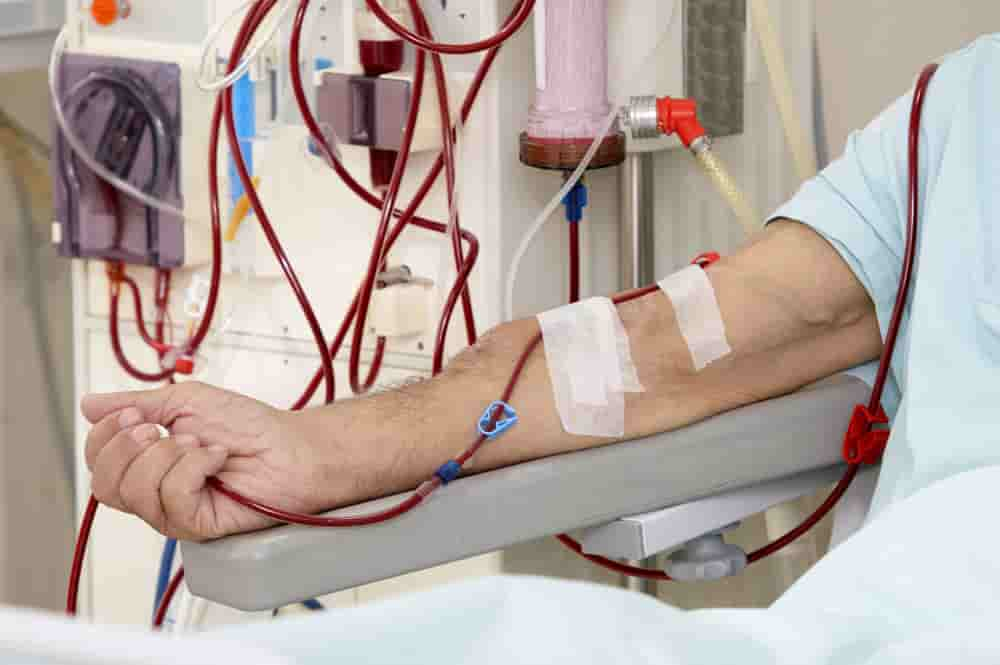
What is Dialysis?
Dialysis is a process in which a patient’s blood is filtered through a particular type of filter. This unique filter helps to remove excess water, minerals, and toxins from your blood. In other words, you can say that dialysis is the treatment of kidney diseases that help to get rid of daily metabolic wastes from our bodies by passing them out from our bodies.
Generally, patients either undergo this process three times a week or for four hours at a time with one night stay in the hospital. Different types of dialysis are available in the market, such as peritoneal dialysis, hemodialysis, hemofiltration, etc. The choice between these therapies depends upon age, medical condition, and ability of the patient to do self-care activities. In this article, we will briefly discuss dialysis.
When you have kidney disease, the blood vessels in your kidneys get damaged. This damage affects the glomeruli, which are responsible for the filtration of excess water, minerals, and toxins from your blood.
Usually, our kidneys filter about 136 to 180 liters of fluid daily. Still, in case of kidney failure, that filtering capacity gets decreased up to 7-10 liters per day, which produces a high level of these metabolic wastes in the body.
So to lower down those excessive wastes, it is essential for patients either to go on dialysis or take some other type of therapy. Dialysis doesn’t cure kidney failure, but it can help delay the complete loss of kidney function by many years.
When you are on dialysis, your blood is passed through a particular type of filter (dialyzer), filled in with different kinds of chemicals to remove excess water, minerals, and toxins from your blood.
This process usually takes about an hour, depending on the machine settings. Generally, two types of filters are available for this process: hemodialysis and peritoneal dialysis.
what is kidney dialysis:
Dialysis is a mechanical method of removing waste and excess water from the blood in people whose kidneys are not usually working. The kidneys act as an internal filter to remove excess water, urea (a toxin), salts (electrolytes), and other wastes. The wastes are removed from the blood by an artificial kidney machine called a dialysis machine. Dialysis can be divided into hemodialysis and peritoneal dialysis.
Need of dialysis:
Dialysis is needed when the kidneys can no longer remove wastes and extra fluid from the body, as in chronic kidney failure. When kidney function declines, harmful levels of fluid, electrolytes, and waste products can build up in your body. This condition is called uremia.
People with kidney disease may first be treated by controlling their diet and using medicine to manage symptoms such as nausea or anemia (low red blood cell count). Dialysis usually begins when a person’s creatinine level reaches 4 mg/100ml.
The patient will go on dialysis until his renal function has improved enough to return home and continue treatment there. A person can also receive hemodialysis at home if they have special equipment.
Monitoring of dialysis:
Dialysis treatments are given several times a week, typically lasting about 3 to 4 hours per session. The patient will lie on his back while the doctor inserts a thin tube called a catheter into a large blood vessel in the chest or arm. This tube is then connected to the dialysis machine, removing waste and extra fluid from the bloodstream.
Blood flows through this tube in one direction only, allowing waste products to be removed along with excess fluid. Blood flow can also be reversed temporarily to remove larger clots or masses during treatment if needed. Dialysis should always be carried out under medical supervision because it involves using tubing that comes directly into contact with your blood.
Conventional dialysis:
Conventional hemodialysis is performed by an artificial kidney machine consisting of a blood compartment, a membrane oxygenator, and tubing to remove waste products. Healthy kidneys can concentrate wastes in the urine to be excreted without extra fluid entering the body. By contrast, the artificial kidney concentrates uremic toxins and water in the dialysate to remove from the blood.
The concentration gradient across the semipermeable membrane oxygenator causes water to diffuse into the blood compartment, treated as excess extracellular fluid.
The higher solute concentrations in blood-side compartments cause urea diffusion and others into these compartments during passage through the membrane oxygenator. The worst problem is an accumulation of urea in the blood compartment, which can result when its diffusion rate through the membrane oxygenator exceeds its removal rate by ultrafiltration.
Types of dialysis:
1. Conventional hemodialysis (regular dialysis)
2. High-flux hemodialysis
3. Slow continuous ultrafiltration (SCUF)
4. Peritoneal dialysis
5. Home hemodialysis
6. Hemodiafiltration and hemoperfusion
Conventional dialysis:
a: in conventional hemodialysis, blood passes through an artificial kidney or dialyzer membrane made up of synthetic fibers that are semipermeable to red blood cells but not to plasma proteins and small molecules such as urea and creatinine.
These substances diffuse from the blood compartment across the membrane into a dialysate solution, forming a concentration gradient that drives their removal from the blood.
b: the dialysate is circulated outside of the patient’s body, where it absorbs urea and other wastes and delivers them to a waste disposal system.
c: During hemodialysis, blood may be passed through a disposable or reusable dialyzer whose exterior is porous plastic and whose interior contains hollow fibers that separate two fluid compartments using semipermeable membranes.
The dialysis solution enters the lumen on one side of each membrane, diffuses into blood across that membrane as described above, then leaves on the other side as dialysate for its trip back to an external reservoir before re-entering circulation via some tubing system.
Dialysis treatment:
blood flows through the dialyzer membrane, diffuses across it to form a concentration gradient, then moves back into circulation by diffusing along that gradient. An equilibrium of sorts is reached during the treatment when the rate at which wastes are removed equals the rate at which they are produced.
Undergoing hemodialysis:
hemodialysis machines have several different sets of tubing attached to them, called access needles or vascular access ports. These needles go either into large veins in your arm or leg or directly into your neck’s artery.
A shorter tube called a catheter is inserted into another vein in your body and left there permanently for ease of access during future treatments. This catheter can be connected to one tubing set for each dialysis treatment.
The dialysis machine, which has the settings of blood pressure on it, is connected to tubing via a large tube called a roller pump. Inside this machine are another fluid compartment and semipermeable membrane but with only one membrane instead of two.
Blood flows through an inlet line and out through an outlet line into and out of this compartment before washing back into the patient’s veins after crossing its semipermeable membrane. The dialysate solution flow rate can be adjusted by changing the speed at which this chamber spins, typically up to 800 RPM (0-2400 RPM available).
What is kidney dialysis:
kidney dialysis is the removal of accumulated wastes in blood using an artificial kidney.
Dialyzer:
A membrane device uses diffusion to separate fluids, proteins, and other particles across a selectively permeable barrier separating two liquids. It consists of hollow fibers through which the blood flows and is separated from dialysate fluid by thin membranes.
Here are two chambers, one for blood and one for dialysate, attached at their ends via hollow tubes or fibers. These tubes can be woven into a large hemodialysis tubing pipe, so blood flow through them becomes more straightforward.
Waste diffuses along their concentration gradient from one chamber to another across the semipermeable membrane, but only when the dialysate fluid flows. this means that blood flow and the movement of waste and dialysate must be carefully matched to avoid clotting or other problems.
The solute level in the dialysate compartment is practically zero since it has been filtered from blood plasma. If not, the net diffusion would be reversed via concentration effects (much like osmotic pressure).
Hepatorenal syndrome (hrs) describes a collection of physical symptoms associated with acute or chronic liver failure that result from decreased blood flow through the kidneys.