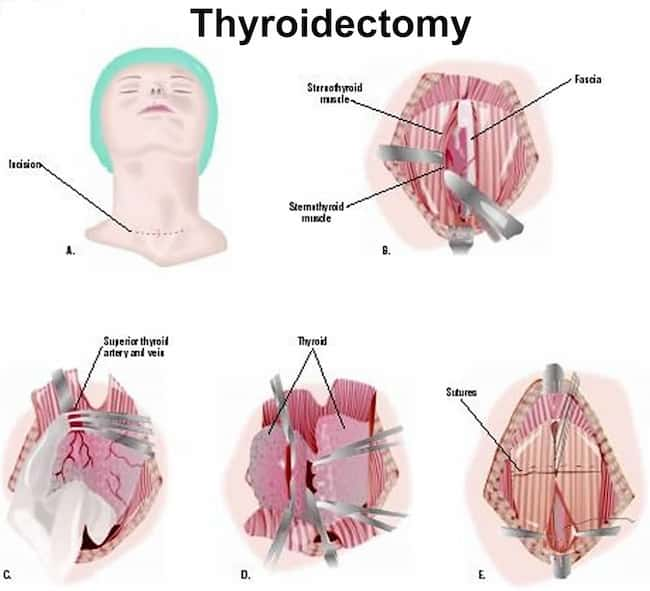
Complications of Thyroid Removal
After removal of the thyroid, complications are expected. The most common ones are infection, hypocalcemia, hyperthyroidism, and damage to parathyroids.
There are four parathyroid glands on the back of the thyroid gland, which controls blood calcium levels. After removing the thyroid gland these glands become inactive and starts producing fewer parathyroid hormones, which is the cause of hypocalcemia after removal of the thyroid gland. This can be countered by taking calcium supplements orally or intravenously.
After removal of the thyroid gland some patients are at risk for developing hyperthyroidism, but this is rare. To prevent this there are two types of treatment, one is to take anti-thyroid medicines like propylthiouracil (PTU) orally for three months and another one is Iodine treatment where the patient takes iodine supplement daily for 90 days until the remaining part of the damaged thyroid heals and starts working.
The most common complication after removal of the thyroid gland is damage to parathyroids (specifically the inferior and superior glands). If damaged, these glands start producing a very high or low level of calcium which causes serious problems for patients’ health. This can be counteracted by regularly monitoring blood calcium levels.
complications of thyroidectomy:
1. hypothyroidism
2. transient or permanent recurrent laryngeal nerve paralysis, which leads to hoarseness of voice and difficulty in swallowing liquids
3. re-operation for bleeding from the suture line
4. injury to trachea/esophagus/ phrenic nerve
5. hemorrhage, infection and wound dehiscence can be seen at the operative site, which may require further surgery/ hospital stay, etc…
1)hypothyroidism:
occurs frequently due to inadvertent damage to the gland during thyroidectomy but may occur even after subtotal thyroidectomy (which has a higher rate of hypothyroidism than total thyroidectomy), as sometimes remnant tissue may be left behind.
– Hypothyroidism is due to insufficient secretion of thyroid hormone, which leads to slowing down of all bodily activities, and hence drowsiness/ obesity/ metabolic syndrome/ glucose intolerance turns into diabetes mellitus, etc…
– Untreated hypothyroidism can cause severe complications like neuropathy (due to demyelination) high cholesterol, coronary artery disease; women may have menstrual irregularities; postmenopausal hot flushes; osteoporosis, later on, may lead to fracture of vertebrae or other bones if they fall.
– Hypothyroidism has also shown an increased risk for the development of breast cancer.
2)recurrent laryngeal nerve paralysis:
– Injury to the recurrent laryngeal nerve is the most common complication of thyroidectomy.
– Patient initially has hoarseness, but with the passage of time loses normal voice, and may even lose the ability to speak (hence emergency tracheotomy may be needed for feeding). Recurrent laryngeal nerves are vulnerable because they lie across the midline in the upper mediastinum, between the esophagus and trachea; all though they cannot be missed during dissection, they can still get injured accidentally.
– If injury (or temporary damage) occurs then recovery depends upon several factors like severity/ location/ duration etc., pain sensitivity especially after surgery plays an important part as this damage is more distressing than other possible injuries during thyroidectomy.
– Residual paralysis may be permanent or temporary, but many can recover full voice within six months of surgery, except for one case study where a patient had complete loss of voice even after 5 years.
3)re-operation for bleeding from suture line:
– Patient has neck swelling due to the slow oozing of blood that forms a clot at the site of operation, called a hematoma. This may occur due to the following reasons:
1] injury to arteries spasm, which stops bleeding initially but later on they start oozing blood slowly giving rise to the neck swelling overtime period.
2] if dissection is difficult surgeon might inadvertently cut through an artery while clamping the thyroid gland.
– Usually, hematoma resolves spontaneously within a week, after which swelling starts reducing and the larynx becomes visible. If there is persistent bleeding then the chances of reopening the wound increase.
4) injury to trachea/esophagus/phrenic nerve:
– Injury to the phrenic nerve causes paralysis of the diaphragm and breathing becomes labored. Injury to other nerves could cause other complications like injury to the trachea, esophagus, etc.
– Other complications:
Banding of thyroid vessels can lead to bleeding from suture line/ surgical wound after surgery, should be treated with cauterization/ligation.
5)haemorrhage/ infection/wound dehiscence:
– Sometimes there may be a lot of postoperative bleeding which requires reopening the wound for control of hemorrhage. If a wound is not closed properly then the patient may have early discharge from the hospital but later on get delayed healing, infection, or wound dehiscence.
6)damage to parathyroid glands:
– Hyperparathyroidism is most common after total thyroidectomy, where it occurs in about 0.5-2% of cases, but when subtotal thyroidectomy is performed for the benign disease this risk is less (0.1%) than when total thyroidectomy is performed for malignancy (3%). A special sign called a “stiff neck” may be seen in patients with parathyroid damage because of restriction of neck movements. Sometimes they also have renal calculi/diarrhea / impaired vitamin D metabolism leading to osteoporosis/ fractures etc., syndrome before surgery.
7) Diplopia:
– Postoperative diplopia may occur due to pressure on the oculomotor nerve during surgery and its severity depends upon the level of injury. If it is mild then symptoms resolve within 1-3 weeks, but if it is severe then ptosis and eyeball retraction occur which may take several months to resolve.
8) tracheoesophageal fistula:
– At times thyroidectomy can result in an abnormal connection between windpipe and gullet, called a tracheoesophageal fistula. This complication mostly complicates pediatric cases rather than adult ones. Postoperative morbidity depends upon the type of injury (mucosal vs. skin), size of the defect, and distance between upper and lower ends.
9)thyroid remnant syndrome:
– It is also known as thyroid bed or collar button, where total removal of the gland is not possible because of its fixation to surrounding structures so the surgeon leaves behind a small volume of thyroid tissue. Also, small pieces may remain attached to the trachea/esophagus causing these complications: destruction by recurrent laryngeal nerve and/or compression by esophageal contractions.
Thyroid removal long term side effects:
1. hypothyroidism & goiter formation:
Hypothyroidism occurs due to damage/ removal of the entire gland or its parts on one or both sides of the neck. It is treated with thyroxine hormone replacement, which has to be taken lifelong for proper growth and development in children since it affects the normal maturation of the brain and other organs.
Goiter can develop if the thyroid gland is destroyed due to another disease process/ toxic iodine excess / autoimmune attack.
2)atrophy of salivary glands:
Salivary glands are very closely related to the tissues lining the upper part of your windpipe (trachea), so they may atrophy following total laryngectomy when the voice box is removed. Since salivary glands are part of the respiratory system, when they atrophy breathing becomes very difficult.
3)hypocalcemia:
Long-term use of thyroid medications can cause elevated calcium levels in your body because these meds contain T4 which gets converted to active T3 form in the liver & kidney. This may cause increased bone density or even osteoporosis if additional calcium supplements are not given.
4)hyperparathyroidism:
Thyroidectomy frequently causes hyperparathyroidism, because parathyroid glands are located close to the thyroid gland so they are often injured during surgery, resulting in damage/ removal of one or more of them. This condition is treated by parathyroid hormone (PTH) replacement.
5)Enterocystoplasty:
When for any reason colon cannot be used in making a pouch, intestines are used instead. It is performed when radiation treatment has destroyed the patient’s rectum and anus. Due to intestinal stoma, some special precautions need to be taken like the preference of low residue diet/ avoiding constipation, etc.
6)strictures after surgery:
There may be stricture of the upper part of the windpipe (trachea), due to scarring at its margins following ENT surgery on the larynx or tracheostomy tube passage. This can be narrowed up completely or partially & may cause airway obstruction. Strictures can occur in scar tissue at the site of the tracheal.
Thyroidectomy complications and management:
1. a) thyrotoxicosis after surgery:
Lack of thyroid hormone may result in thyrotoxicosis which can be managed by taking medication containing small doses of thyroid hormones. T3 & T4 are used most often, but since these hormones have a short half-life their effect is lost once treatment is stopped. Individuals with thyrotoxicosis due to surgical removal of the gland have to take these medications for a prolonged period or even lifelong.
2 b) hypothyroidism after surgery:
Hypothyroidism results when the entire gland/part on one or both sides of the neck is removed, even if it is done surgically. Although early postoperative complications like hypocalcemia can be managed by taking calcium supplements, if thyroid tissue is destroyed due to another disease process, autoimmune attack, or toxic iodine excess, hypothyroidism results.
2 c) postoperative complications:
Complications after surgery include throat infection, bleeding from veins left behind in the neck, airway obstruction due to tracheal stenosis, damage to nerves controlling vocal cord/swallowing muscles, etc.
3 d) stomal stenosis following surgery:
Stomal stenosis can also occur as a result of strictures formation at the margins of the stoma opening. This causes narrowing & complete blockage of the stoma lumen which causes further development of constrictive bronchitis. Constrictive bronchitis is a condition caused by scarring at the opening of the upper part of the windpipe (trachea), which narrows down air passage and causes difficulty in breathing. It can be treated by dilation of stoma lumen & stomal dilatation.
4 e) problems following surgery:
Problems that may occur after surgery include salivary gland atrophy, thyroid hormone imbalance, bone density deficiency due to hypocalcemia, etc.
5 f) postoperative care:
Most ENT surgeries are resumed within 2 weeks so the patient is generally discharged within this period postoperatively with some precautions like avoiding strenuous work/ exercises/ lifting heavy objects etc.
The choice of diet depends on stoma which is also taken into account. Speech therapy may be advised due to postoperative laryngeal/cricopharyngeal paralysis if vocal cord nerve paresis occurs during surgery.