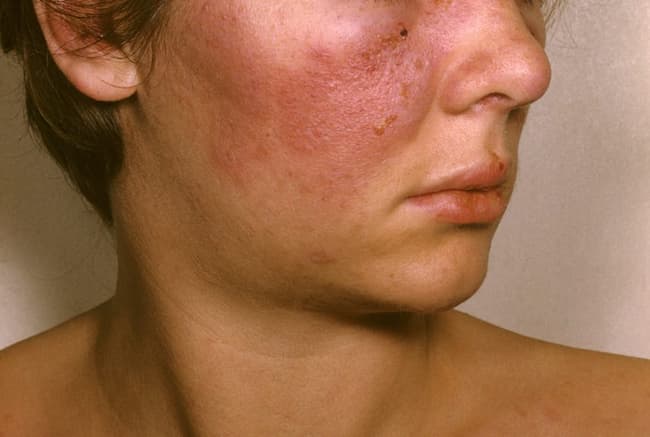
Lupus Erythematosus
An autoimmune disease in which the body’s immune system mistakenly attacks healthy tissues and organs.
The leading cause of lupus is not known, but it can be triggered by environmental factors such as:
extreme sun exposure, cigarette smoke, certain drugs (such as procainamide), and infectious organisms like viruses or bacteria. Other factors may include genetics, hormones, stress, and diet.
Lupus nephritis:
A type of kidney disorder caused by lupus that affects men and women equally. Most cases are mild to moderate yet disabling with severe consequences, including frequent infections accompanied by fever and abdominal tenderness. It usually appears suddenly without warning signs. If left untreated, it can lead to death via internal bleeding, condition, or kidney failure.
There is no known cause for this disease; there have been few medical advancements to cure this disorder. However, with the help of steroids and painkillers, we can at least manage it and ease some discomfort that comes along with it.
As mentioned above, lupus nephritis is merely a mild to a moderate kidney disorder that can lead to severe consequences. Unfortunately, it turns out that there is no specific test for diagnosing the presence of the disease in either rats or humans; this leads us to have little scientific evidence which might explain how this disease progressed, like what happened with our rat Ajax.
It seemed as if he had an infection or something similar, but red spots started to appear on his pink skin, and soon after, they spread all over his body, especially near his ear and hind legs which seemed most severely affected by this disease.
Seeing how every day you would clean him up and reduce the effect of fleas was just incredible; you will have a significant contribution towards finding treatment for this condition in rats because you have witnessed how much a rat suffers when they have lupus nephritis.
At first, we thought that the symptoms were from an allergy to the bedding but soon realized that it was not mosquito bites or fleas because he would be scratching himself raw, and there was no initial swelling of the skin, which indicated parasites. Instead, we could see red spots appearing on his skin within 24 hours of being bitten by mosquitoes.
The only logical explanation for us is that it may be a disease since Ajax had never been exposed to any other rat with this condition, nor did we know anyone who owned a pet rat before. However, there are chances that our rat might have come across it in his previous environment.
We have watched his condition worsen over time, concluding that this is not a virus or secondary effect of another disease. Still, possibly an autoimmune disorder, in much the same way lupus affects humans.
It only came about when he was approximately six months old, which is why we believe that it may be genetic in origin, seeing how both Ajax’s parents are also affected by the same ailment, albeit much less severely than him.
Lupus erythematosus treatment:
Steroids for short term control of symptoms, also used in severe cases
Immunomodulators azathioprine and methotrexate suppress the immune system and can be lifelong treatments. They are the first-line treatment in lupus nephritis (kidney involvement)
Cyclophosphamide:
this is a chemotherapy drug that destroys your immune system. It is usually given as an injection over three days every three months. This treatment needs to continue for life, but you will recover your normal immunity within six weeks after stopping it.
You may need cyclophosphamide if you have very high blood pressure resulting from kidney damage or a non-renal disease not controlled by other drug treatments.
Renal biopsy:
A small sample of the kidneys is removed to be looked at under the microscope to see how damaged they are. This is usually done when your creatinine levels rise steadily over time, but you don’t have any symptoms of kidney disease. Your nephrologist (kidney doctor) may recommend that you have this procedure if your level of protein in your urine is high or if there’s blood in your urine.
Systemic lupus:
A lupus diagnosis is made by examining the blood under a microscope and looking for antibodies that react to double-stranded DNA, which is only present in the nuclei of cells. Antibodies can be measured through serum tests or urine analysis. The antibody test does not prove that you have SLE, but rather that your immune system has begun producing these antibodies because something (the disease) is causing it to do so.
These autoantibodies also distinguish lupus from most other diseases, which usually do not affect more than one organ system (a characteristic known as multicentricity).
Therefore, having positive ANA or anti-dsDNA antibodies can strongly suggest an individual has SLE; however, they are neither necessary nor sufficient in themselves to make a diagnosis.
The only tests that confirm SLE are the kidney biopsy and anti-nuclear antibodies in the patient’s serum.
Autoantibodies may be present in patients without SLE, although they are usually absent in healthy individuals.
Lupus erythematosus symptoms:
1. malar rash (a “butterfly rash” across both cheeks)
2. discoid rash (red, raised patches of skin that sometimes blister or peel; usually occurs on the face, neck, and chest)
3. photosensitivity (sensitivity to sunlight; may increase the tendency for skin lesions and rashes to appear)
4. alopecia (hair loss; can be patchy or complete)
5. Raynaud’s phenomenon (unusually decreased blood flow through the fingers causes them to cool in cold weather or become painful when exposed to cold after being warm, most commonly appearing in women ages 20-40 years old.)
6. oral ulcers
7. arthritis of multiple joints (affecting hands, wrists, knees, and feet)
8. muscle weakness
9. loss of memory or impaired concentration
10. psychiatric symptoms such as depression or psychosis
11. serositis (inflammation of the membranes that line the lungs and heart; pleurisy, pericarditis)
12. renal disease (kidney inflammation or scarring that can lead to chronic kidney failure), which is seen in up to half of all individuals with SLE during their lifetime
13. hematological abnormalities such as lymphopenia, leukopenia, thrombocytopenia, hemolytic anemia, or blood clotting disorders
14. hypothyroidism (thyroid gland does not produce enough thyroid hormone)
15. platelet aggregation abnormalities
16. neurologic symptoms such as seizures and psychosis
17. vascular problems leading to either bleeding or impaired blood flow, which can cause either ischemic attacks (lack of blood flow to parts of the body) or thrombosis (blood clots obstructing blood vessels)
18. vasculitis (inflammation inside the walls of arteries and veins, damaging the blood vessel wall), which may be very serious if it affects a vein in, for example, the brain
19. anemia from “autoimmune hemolytic anemia.”
20. aortic root dilation, a complication that can lead to regurgitation or stenosis of the aortic valve
Lupus treatment:
1. Sunscreen and protective clothing may help to prevent or limit skin rashes.
2. Corticosteroids such as prednisone are often taken for a long time, based on the severity of symptoms and how quickly they improve with treatment. In general, oral corticosteroids are not used immediately in lupus because these medications can worsen kidney problems from autoantibodies attacking proteins in your kidneys.
3. Immunosuppressants such as azathioprine (Imuran) and mycophenolate mofetil (CellCept) may be prescribed in cases where disease-modifying antirheumatic drugs (DMARDs) do not work well enough or when you have more severe disease.
4. Antimalarial drugs such as hydroxychloroquine (Plaquenil), chloroquine (Aralen), or quinacrine may be prescribed to some patients with lupus, usually when the drug Sulfasalazine is not helpful enough. These medications can help prevent flares of the disease.
5. Corticosteroids are often combined with immunosuppressants because they work well together, and neither one alone works for every patient. This combination helps treat people with more severe cases of lupus who have organ damage from uncontrolled inflammation and frequent flares, anemia, low platelet counts, a weak immune system, a need for a large number of oral steroids, or a high risk of severe complications from lupus.
6. Antimalarial drugs, used alone or combined with corticosteroids, can also be helpful in severe cases of lupus that do not respond to other medications. However, these drugs do have side effects, and they are less likely to work on people with renal disease or blood vessel damage caused by lupus.
7. Immunosuppressants such as cyclophosphamide (Cytoxan) and mycophenolate mofetil can help treat lupus that does not respond to other treatments or is causing severe organ damage
8. High-dose intravenous immunoglobulin therapy may be an option for some people with lupus who have a particular type of antibody called a “nuclear antibody” and have kidney, lung, or central nervous system disease. This treatment can suppress the autoimmune response temporarily by removing antibodies from your blood.
9. Therapies designed to suppress your immune system are called immune suppression therapy, and these medications include azathioprine, cyclophosphamide, methotrexate, tacrolimus (Prograf) cyclosporine (Sandimmune, Neoral), sirolimus, mycophenolate mofetil, belatacept (Nulojix), or rituximab.
Cancer chemotherapeutic agents are also used to suppress the immune system of lupus patients. Medications that modulate your immune system are called immunomodulatory, and these include hydroxychloroquine, leflunomide (Arava), teriflunomide (Havrix), or parenteral gold.
1O. In some cases, surgical procedures may be necessary, including coral transplants for dry eyes, corneal transplants for severe eye damage, or amputations of affected limbs.